In Canada between 2002 and 2016 there were an estimated 235,471 head injuries, with 22.6% receiving a traumatic brain injury (TBI) diagnosis (Injury in Review, 2020). The numbers reported are expected to be only a fraction of the ones sustained. As many injured people do not seek appropriate medical care, brain injuries have been referred to as a silent epidemic and are a leading cause in disability, mortality, and morbidity (Alkhaibary et al., 2021). Brain injuries can occur for a multitude of reasons, some of the most common being; motor vehicle accidents, contact sports, violence, strokes, tumors and infections.
Types of Brain Injuries
Acquired Brain Injury (ABI)
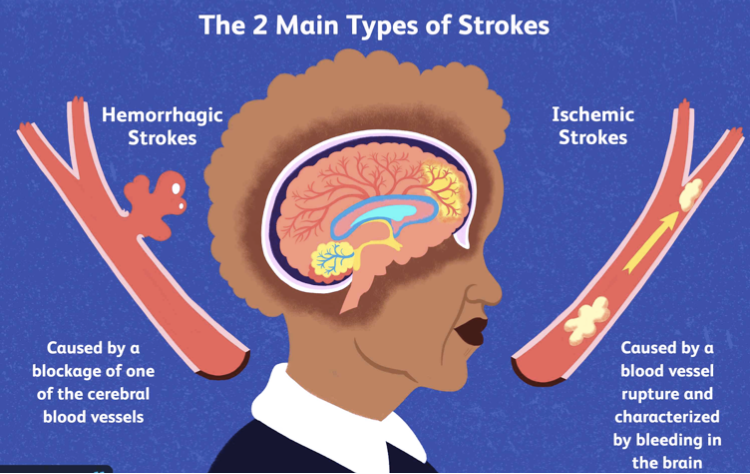
Strokes or cerebrovascular accident (CVA) occur when cerebral perfusion of vasculature has been compromised (Khaku & Tadi ., 2021). Strokes can be either ischemic or hemorrhagic, in ischemic stroke the brain is compromised by a blockage that was developed elsewhere in the body (embolic) or within the brain (thrombotic). On the other hand, hemorrhagic strokes occur when a blood vessel has ruptured, injuries can be subarachnoid hemorrhage or intracerebral hemorrhage (Unnithan & Mehta., 2022).
Brain Tumors are rare and account for approximately 3% of all cancer diagnosis worldwide, brain tumors are defined as malignant or benign (Miranda-Filho et al., 2016). ABI’s may result after brain tumor diagnosis due to increased intracranial pressure and/or surgical treatments.
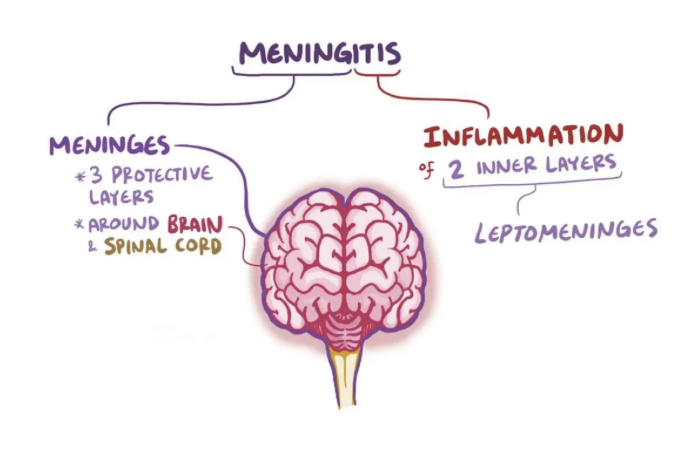
Infections such as bacterial meningitis can impact the brain in several ways which can have serious long term consequences that can leave an individual with an ABI.
Traumatic Brain Injuries (TBI)
TBI’s are a form of ABI that are characterized by primary and secondary injuries to the head. Primary injuries are external forces that cause injury, secondary injuries comprise injuries sustained minutes to days from the initial trauma (Alkhaibary et al., 2021). A TBI’s severity is categorized based on defined criteria known as the Glasgow Coma Scale (GCS). The GCS has 3 classifications for head injuries; mild, moderate, or severe.
Mild TBI (mTBI) are often referred to as concussions, this type of TBI involves a direct blow to the head which causes acceleration/deceleration of the head (Georges, 2022). Those with mTBI may present with confusion or loss of consciousness (Georges, 2022). Although mTBI’s are less severe, repeated mTBI can have serious consequences. For example, Rowan’s Law (Concussion Safety, 2018) was implemented in Ontario sports after 17 year old Rowan Stringer died due to sustaining multiple concussions at a soccer tournament in May 2013 (Ontario, 2022). Rowan’s Law provides education to coaches, parents, and students on the signs and symptoms of concussions, placing emphasis on not pressuring athletes to continue playing after sustaining a concussion.
Those with Moderate-Severe TBI may lose consciousness for up to 30 minutes or more, and can be diagnosed based on tools such as CT scans (Malec., 2007). Types of moderate-severe TBI include; epidural hematoma, subdural hematoma, contusions, subarachnoid hemorrhage, intracerebral hemorrhage, and diffuse axonal injury.
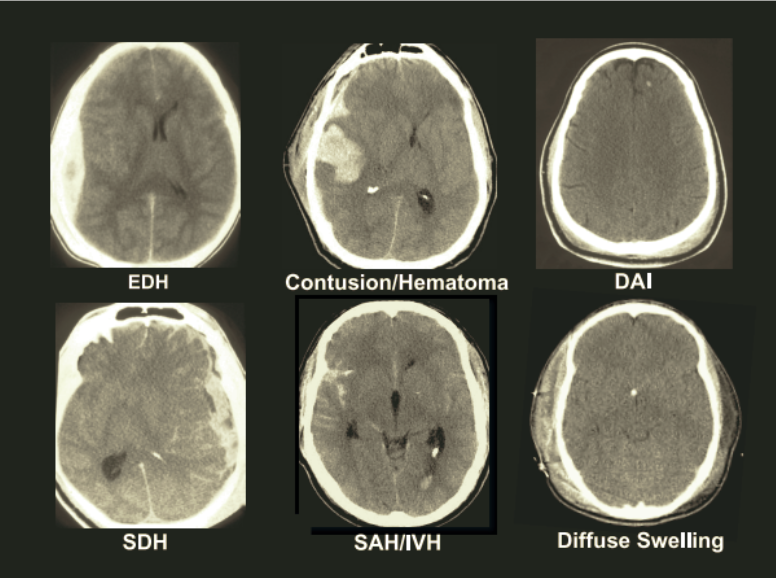
Epidural hematomas (EDH) occur when an artery ruptures between the skull and dura mater that causes intracranial pressure. EDH takes place most commonly after a skull fracture, about 85%-95% of cases (Tenny & Thorell., 2022). Subdural hematomas (SDH) happen when blood pools between the dura and arachnoid mater that causes intracranial pressure. Contusions of the brain can be a result of coup or contrecoup types. As demonstrated in Figure 1 coup types result in contusions where the sight of impact occurred. Whereas contrecoup types occur on the contralateral side where the impact occurred. As mentioned above, Subarachnoid hemorrhages (SAH) result when a blood vessel ruptures between the space in arachnoid and pia mater, SAH’s are mostly commonly caused by aneurysms or trauma (Ziu & Mesfin. 2021). Intracerebral hemorrhage (ICH) occurs when a hematoma is present within the brain parenchyma that leads to major blood loss, ICH’s make up 10-20% of strokes, yet may result from trauma (Tenny & Thorell., 2022). Diffuse Axonal Injury (DAI) takes place with axonal shearing from acceleration/deceleration injuries (Galango et al., 2017).
References
Alkhaibary A, Alshalawi A, Althaqafi R M, et al. (May 29, 2021) Traumatic Brain Injury: A Perspective on the Silent Epidemic. Cureus 13(5): e15318. DOI 10.7759/cureus.15318
Galgano M, Toshkezi G, Qiu X, Russell T, Chin L, Zhao LR. Traumatic Brain Injury: Current Treatment Strategies and Future Endeavors. Cell Transplant. 2017 Jul;26(7):1118-1130. doi: 10.1177/0963689717714102. PMID: 28933211; PMCID: PMC5657730.
Holm L, Cassidy JD, Carroll LJ, Borg J. Summary of the WHO collaborating centre for neurotrauma task force on mild traumatic brain injury. Journal of Rehabilitation Medicine. 2005;37(3):137–141.Holm L, Cassidy JD, Carroll LJ, Borg J. Summary of the WHO collaborating centre for neurotrauma task force on mild traumatic brain injury. Journal of Rehabilitation Medicine. 2005;37(3):137–141.
Khaku AS, Tadi P. Cerebrovascular Disease. [Updated 2021 Sep 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430927/
Minister’s year Three progress report on Rowan’s law (concussion safety), 2018. ontario.ca. (n.d.). Retrieved April 26, 2022, from https://www.ontario.ca/page/ministers-year-three-progress-report-rowans-law-concussion-safety-2018
Release Notice – Injury in Review, 2020 Edition: Spotlight on Traumatic Brain Injuries Across the Life Course. Avis de publication – Étude des blessures, Édition 2020 : Pleins feux sur les traumatismes crâniens tout au long de la vie. (2020). Health promotion and chronic disease prevention in Canada : research, policy and practice, 40(9), 294. https://doi.org/10.24095/hpcdp.40.9.05
Saatman, K. E., Duhaime, A. C., Bullock, R., Maas, A. I., Valadka, A., Manley, G. T., & Workshop Scientific Team and Advisory Panel Members (2008). Classification of traumatic brain injury for targeted therapies. Journal of neurotrauma, 25(7), 719–738. https://doi.org/10.1089/neu.2008.0586
Tenny S, Thorell W. Intracranial Hemorrhage. [Updated 2022 Feb 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470242/
Unnithan AKA, Mehta P. Hemorrhagic Stroke. [Updated 2022 Feb 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559173/
Ziu E, Mesfin FB. Subarachnoid Hemorrhage. [Updated 2021 Aug 9]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK441958/
Images:
https://www.google.com/url?sa=i&url=https%3A%2F%2Fen.wikipedia.org%2Fwiki%2FCoup_contrecoup_injury&psig=AOvVaw1Z0q_yXd6mLfnaoFVkNVOb&ust=
1651012014693000&source=images&cd=vfe&ved=0CA0QjhxqFwoTCLjKlKihsPcCFQAAAAAdAAAAABAD
https://www.google.com/url?sa=i&url=https%3A%2F%2Fwww.osmosis.org%2Flearn%2FMeningitis&psig=AOvVaw04bH6PzVYagla_qt_Tohig&ust=
1651079508873000&source=images&cd=vfe&ved=0CAwQjRxqFwoTCPiCh9ScsvcCFQAAAAAdAAAAABAJ


